Climate Change and Health Vulnerability Assessments
Introduction
Climate change and population health are intrinsically intertwined. The impacts of climate change on health, safety and well-being are extensive and wide-ranging. These impacts include fatalities and injuries due to severe storms, landslides and floods; an increase in infectious diseases, including those from water-borne pathogens; heat-related illness and respiratory and cardiovascular disorders; increased UV exposure; and the long-term mental health impacts from extreme weather events. In addition, indirect impacts from extreme weather events on transport and access routes can have significant implications in relation to access to employment, food and other services. Those who are already disadvantaged, through existing long-term illness or disability, low income or other social disadvantage, are likely to be disproportionately affected. Climate Change and Health Vulnerability Assessments (CCHVAs) are grounded at the intersection of public health and the environment. They aim to identify the future trajectory of climate change and related impacts and the potential health impacts due to the changing climate. In addition, CCHVAs identify the most vulnerable sub-groups within a population who might be disproportionately impacted in the short, medium and long-term, as well as the inherent resiliencies within a population to withstand the impacts of climate change. This information then informs the recommendation of adaptation strategies to either build upon or develop new resiliencies to combat the impacts of climate change and preserve health and wellbeing.
The Assessment of Vulnerabilities
Vulnerable communities and peoples are disproportionately affected by climate change impacts, whether this vulnerability is related to low income, poor health, education, ethnicity and/or location. Vulnerable communities can also have more challenges in recovering from climate impacts, especially flooding. In addition, it is also increasingly clear that intersectional differences, including gender, age, Indigeneity, socio-cultural differences, including language and ethnic origin, etc., may amplify or affect how climate change impacts human health and how information and services to mitigate these impacts are accessed. Using a Gender-Based Analysis Plus (GBA+) lens when assessing vulnerability to climate change improves understanding of disproportionate impacts and allows the project team to recommend adaptation strategies to mitigate these differences and minimize the compounding impacts.
Climate Change and Health Vulnerability Assessment of the Northwest Territories (NWT)
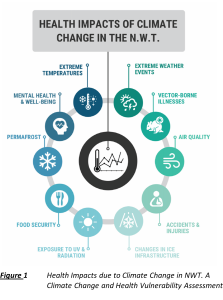
Intrinsik recently collaborated with our partners specializing in climate science to complete a CCHVA of the Northwest Territories (NWT) for the Government of Northwest Territories (GNWT) (March, 2021). The approach and methodology used in the assessment involved the identification of ecoregions in the NWT; current sociodemographic (including assessment of vulnerable populations) and infrastructure conditions; current and future climate change and health impacts; and resiliencies and proposed adaptation strategies. Our project team used three main elements to guide the assessment of potential health impacts due to climate change in the NWT: (1) Adapted methodology of the Climate Change and Health Toolkit by the Ontario Ministry of Health and Long-Term Care; (2) Information gathered from interviews with seven subject matter experts; and (3) Information gathered from a review of academic and grey literatures. The assessment identified the major current and future potential health impacts due to climate change as seen in Figure 1, and also emphasized the disproportionate impacts on the health of vulnerable populations.
 An underlying core of the assessment of health impacts was to identify vulnerable population groups who would, currently and in the future, experience disproportionate health impacts. Although this is not a conclusive list, we focused on the nature of disproportionate impacts to Indigenous communities (who comprise just over half the population of NWT), the elderly, children and youth, women, lower income and those experiencing homelessness, LGBTQ2+ individuals and refugees. It should also be noted that there is considerable overlap between individual vulnerable groups, an example of which is elderly Indigenous women experiencing low income or homelessness.
An underlying core of the assessment of health impacts was to identify vulnerable population groups who would, currently and in the future, experience disproportionate health impacts. Although this is not a conclusive list, we focused on the nature of disproportionate impacts to Indigenous communities (who comprise just over half the population of NWT), the elderly, children and youth, women, lower income and those experiencing homelessness, LGBTQ2+ individuals and refugees. It should also be noted that there is considerable overlap between individual vulnerable groups, an example of which is elderly Indigenous women experiencing low income or homelessness.
Indigenous Peoples and Climate Change
Indigenous peoples in Canada face systemic health inequities and poorer health outcomes, primarily due to long-standing socioeconomic inequities, which are a result of the ongoing legacy of colonialism, the inter-generational trauma of residential schools and inequities in access to health services. Under such circumstances, climate change acts as a risk magnifier, further exacerbating poor health conditions among vulnerable populations by disturbing the balance of the determinants of health.
For Indigenous peoples in the North, the Canadian Arctic has been and will continue to be an area of intense climate change-related impacts. The communities that live there, and especially in the remote regions, demonstrate a high degree of resilience and adaptation even in the face of long-standing health and socioeconomic inequities. Where possible, CCHVAs should build upon and learn from these resiliencies and recommend adaptation strategies that are grounded in the communities’ needs and realities.
For more information on how Intrinsik can help your company, please contact .
Intrinsik Blogger: Dr. Faiza Waheed

